Anatomy:
FemoroAcetabular Impingement (FAI) is a hip condition that is characterised by pain with hip motion as a result of premature contact between the femur (thigh bone) and acetabulum (hip socket). The hip joint is a ball and socket joint, which enables a large range of joint mobility. The acetabulum has a ring of cartilage called the labrum, which deepens the socket and provides stability to the hip joint.

FAI involves an alteration to the anatomy of the hip joint due to bone thickening around the ball of the femur. There are two types of morphology associated with FAI:
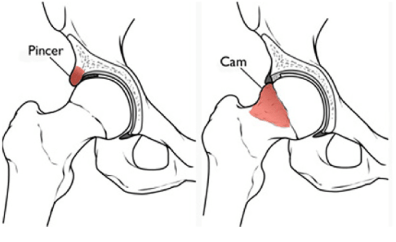
- Cam morphology which is characterised by a misshaped of the femoral head near the femoral neck junction.
- Pincer morphology which is characterised by an “overcoverage” of the femoral head by the acetabulum in which the acetabular rim is extended beyond the typical amount.
- A combination of both morphologies is also possible


The changes associated with FAI are believed to be fairly common. A study by Wall et al. in 2016 found that approximately 30% of the general population had some degree of morphology without necessarily suffering from symptoms. However, both types of morphology can be detrimental to the articular cartilage of the hip joint and the labrum. Due to a large proportion of the general population with hip morphology being asymptomatic, other factors are required for true diagnosis of FAI. Weakness of deep hip muscles is associated with FAI, as this could compromise hip stability and also alter the biomechanics of the hip joint by allowing the femoral head (ball of joint) to slide forwards into the socket and thus causing an overload on the hip joint.
Symptoms:
- Hip and/or groin pain related to certain hip positions or movements.
- Occasionally thigh, back or gluteal pain.
- Stiffness, restricted joint mobility, clicking, catching, locking or giving way of the hip joint.
Conservative Management:



Improving the muscular strength and function of the hip is the main goal of conservative management for FAI. Strength training focuses on addressing weakness of the deep hip musculature – in particular the deep hip external rotators, abductors and flexors – and a subsequent increase in the dynamic stability of the hip joint. Achieving increased strength levels in symptomatic FAI decreases the loading of the labrum thereby decreasing painful symptoms.



A strengthening program should be tailor made for your particular morphology, mechanics and strength deficits. Releasing surrounding musculature will not only help to reduce secondary pain, but also enable the muscle to appropriately activate to encourage strength. According to Griffin et al (2016), symptoms of FAI syndrome will worsen if no treatment is provided. If hip pain is a concern for you and is hindering your mobility and ability to work or play sports, why not contact your physiotherapist today for a consultation?
- Wall PD, Dickenson EJ, Robinson D, Hughes I, Realpe A, Hobson R, Griffin DR, Foster NE. Personalised Hip Therapy: development of a non-operative protocol to treat femoroacetabular impingement syndrome in the FASHIoN randomised controlled trial. Br J Sports Med. 2016;50(19):1217-23.
- Casartelli NC, Maffiuletti NA, Bizzini M, Kelly BT, Naal FD, Leunig M. The management of symptomatic femoroacetabular impingement: what is the rationale for non-surgical treatment? Br J Sports Med. 2016 May;50(9):511-2.
- Griffin DR, Dickenson EJ, O’Donnell J, Agricola R, Awan T, Beck M et al. The Warwick Agreement on femoroacetabular impingement syndrome (FAI syndrome): an international consensus statement. Br J Sports Med. 2016; 50(19):1169-76.

